Safe Swallowing.
Feeding Tube Clearance.
Ensure your loved one can safely eat, drink, and communicate. We provide expert clinical swallowing evaluations to prevent complications and safely guide NGT or tracheostomy removal.
What is a Clinical Swallowing Assessment?
After a stroke, traumatic brain injury, or prolonged ICU intubation, the complex muscles required for swallowing often become weak or uncoordinated. This condition, called Dysphagia, carries a severe risk of aspiration—where food or liquid enters the lungs instead of the stomach, potentially causing life-threatening pneumonia.
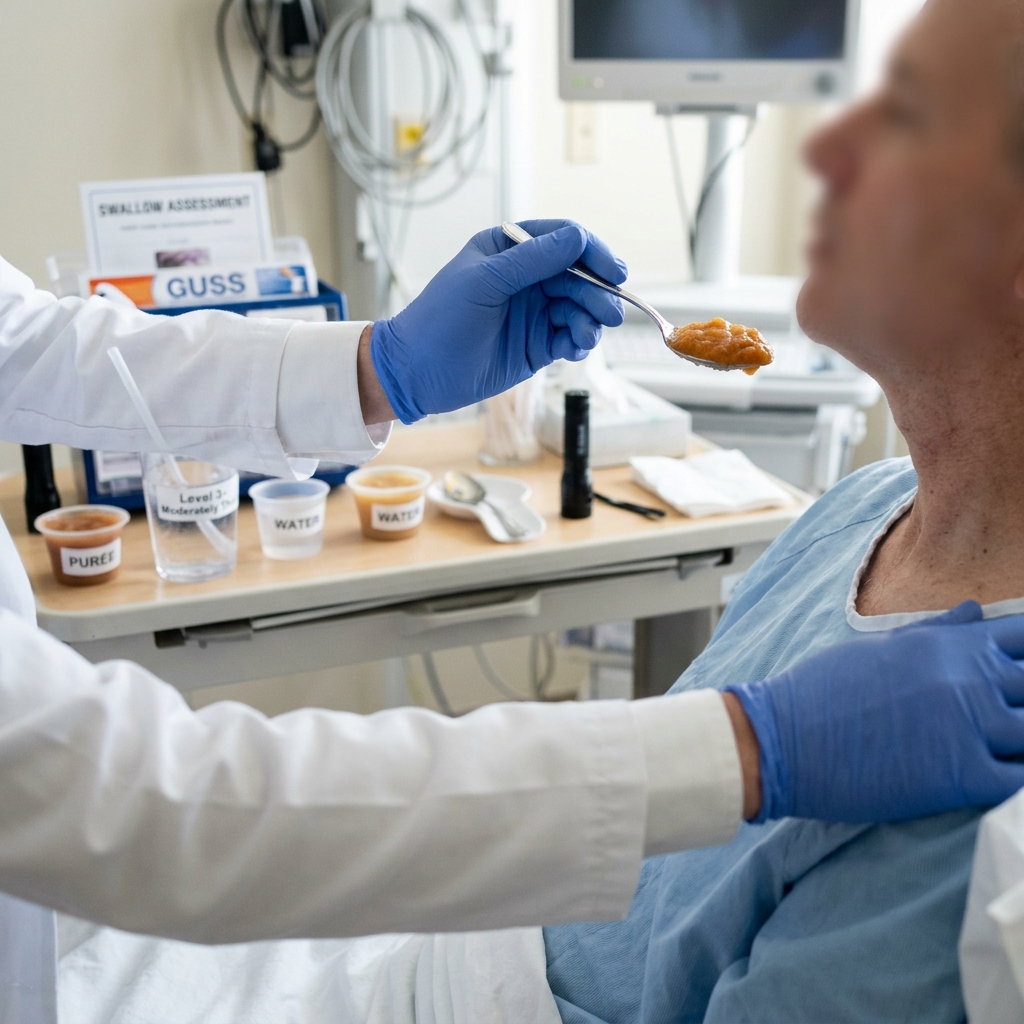
To ensure patient safety, Dr. Rabara performs a functional clinical swallowing evaluation, utilizing protocols like the Gugging Swallowing Screen (GUSS). By carefully observing the patient's ability to process different textures—from pureed foods to thick liquids and regular water—we can objectively determine their exact swallowing capability without immediately requiring invasive equipment.
Who Requires a Swallowing Assessment?
Signs of
Swallowing Impairment
Often, swallowing difficulties are not obvious. 'Silent aspiration' can occur without outward choking, making a professional clinical evaluation critical for your loved one's safety.
Ideal indications
Frequent coughing or 'gurgly' voice during or after meals.
Current NGT or PEG tube dependence wishing to transition to oral eating.
Tracheostomy tube in place requiring clearance for decannulation.
Unexplained weight loss or recurrent respiratory infections.
Clinical precautions
Patient is medically unstable or unable to remain alert for evaluation.
Suspected structural esophageal blockage (requires GI referral).
Acute respiratory distress requiring immediate emergency intervention.
The Realities of
Swallowing Recovery
Restoring a patient's ability to eat independently is our primary functional goal, but safety dictates our timeline:
No Premature Removals
Removing an NGT or tracheostomy before airway reflexes are secure can result in fatal respiratory complications.
Progressive Rehabilitation
Swallowing is a complex muscular coordination. Recovery is rarely instantaneous and requires dedicated therapy effort.
In-Depth Clinical Science
Technical documentation for medical colleagues and analytical patients regarding swallowing pathophysiology.
Explore the Clinical Science: The Pathophysiology of Post-Stroke Dysphagia
The neuroanatomical coordination required for a safe swallow involves over 30 pairs of muscles and multiple cranial nerves. Stroke or TBI disrupts cortical control over these voluntary movements.
The scientific concern is 'silent aspiration', where food enters the lungs without a cough reflex, leading to aspiration pneumonia—a leading cause of post-stroke mortality.
Advanced Indications: GUSS-ICU & Post-Extubation Protocols
Following mechanical ventilation, patients often suffer from 'post-extubation dysphagia'. The physical presence of a tube desensitizes the laryngeal mucosa while muscle disuse leads to atrophy.
We monitor for clinical red flags such as 'wet voice' quality and reduced hyolaryngeal excursion to prevent recurrent ICU readmission.
Detailed Anatomical Review: The 4 Stages of a Safe Swallow
We evaluate the Oral Preparatory, Oral Transport, Pharyngeal, and Esophageal phases. The Pharyngeal phase is the 'point of no return' where vocal cords close—this must happen in less than one second.
Clinical Swallowing & Recovery Guides
Expert resources on recovering from dysphagia, managing feeding tubes, and preventing aspiration pneumonia.
Causes of Choking in the Elderly: Dysphagia & Aspiration Pneumonia
Educate on the Silent Threat: how food slips into lungs without coughing, causing fatal pneumonia.
Stroke & Parkinson's Swallowing Problems: Oropharyngeal Dysphagia
The 'Broken Traffic Light' framework: why neurological signals to the throat fail during disease.
How to Remove an NGT Feeding Tube: Safe Swallowing for Stroke Patients
The emotional grief of tube feeding and the clinical roadmap to graduating back to real food.
FEES & Barium Swallow Tests Explained: The Swallow Test Procedure
Demystifying diagnostics: the difference between X-ray video and endoscopic cameras.
Speech Therapy for Dysphagia: Swallowing Exercises & Rehabilitation
Pivoting perception: how an SLP acts as a 'throat mechanic' to rebuild the reflexive swallow.
Dysphagia Swallow Test Cost & Assessment Clinic in Vigan
Absolute financial transparency and conversion for the elite diagnostic destination in Ilocos Sur.
Laging Nabulunan at Hirap Lumunok? Sintomas ng Dysphagia
Relatable symptom checking for local families: explaining how 'tubig napupunta sa baga'.
Bakit Hindi Makalunok ang Na-Stroke? Paano Tanggalin ang Tubo sa Ilong
Hope and a clinical pathway for stroke survivors to safely transition off the NGT tube.
Magkano ang Swallow Test? (Doktor sa Lalamunan at Dysphagia sa Vigan)
Direct guidance on pricing and booking for Northern Luzon families.
The 3-Step Process
Clinical Bedside Evaluation
We conduct a thorough, step-by-step assessment of the patient's oral motor control and swallowing reflexes.
Diagnostic Coordination
If necessary, we seamlessly coordinate advanced endoscopic testing (FEES) with PhilHealth-accredited ENT specialists.
Targeted Action Plan
We issue a formal medical directive for either progressive therapy or safe apparatus removal.